Diabetic Ulcer Treatment with LED Light Therapy
Diabetic foot ulcers affect approximately 15% of diabetes patients during their lifetime. Wound Blaster uses triple-wavelength pulsed LED technology to increase local circulation, supporting faster wound closure through nitric oxide release and enhanced blood flow.

Understanding Diabetic Ulcers
A serious complication that demands better solutions
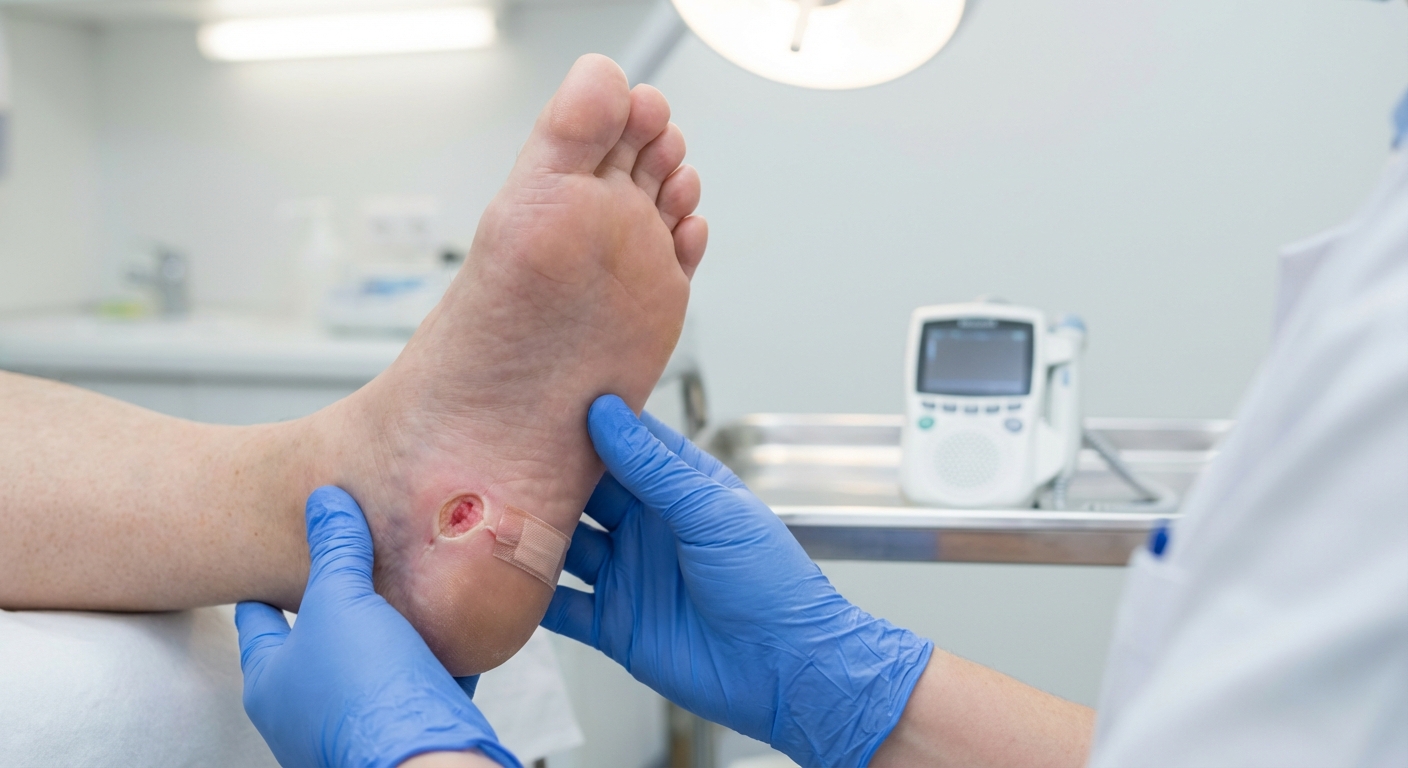
Diabetic ulcers develop when high blood sugar damages nerves and blood vessels, particularly in the feet. Reduced circulation means less oxygen and fewer nutrients reach the wound site, slowing the body's natural healing process. Traditional treatments often involve wound debridement, dressings, off-loading, and lengthy recovery periods.
How Wound Blaster Addresses Diabetic Ulcers
Wound Blaster targets the root cause of slow healing in diabetic wounds: compromised blood flow. Using three therapeutic wavelengths, it stimulates the natural release of nitric oxide to restore circulation.
Light Penetrates Tissue
Infrared, red, and blue wavelengths penetrate several centimeters into soft tissue surrounding the ulcer.
Nitric Oxide Released
Photochemical stimulation of hemoglobin triggers the local release of nitric oxide, the body's natural vasodilator.
Blood Flow Increases
Blood vessels dilate, restoring oxygen and nutrient delivery to the compromised wound site.
Wound Closure Accelerates
Enhanced circulation supports the body's natural wound closure processes, including new capillary formation (angiogenesis).
Who Is at Risk for Diabetic Ulcers?
Recognizing risk factors early is key to prevention and better outcomes
Peripheral Neuropathy
Loss of sensation in the feet makes it difficult to detect injuries, blisters, or pressure points that can develop into ulcers.
Poor Circulation
Peripheral arterial disease (PAD) reduces blood flow to extremities, depriving wounds of the oxygen and nutrients needed for healing.
Uncontrolled Blood Sugar
High blood glucose levels impair the immune system and slow healing processes, increasing infection risk.
Prior Ulcer History
Patients with a history of foot ulcers have up to 65% recurrence rate within 5 years without preventive care.
Foot Deformities
Structural changes like hammertoes, bunions, or Charcot foot create pressure points that increase ulcer risk.
Lifestyle Factors
Smoking, obesity, and a sedentary lifestyle further compromise circulation and healing ability.
A Better Approach to Diabetic Ulcer Care
Wound Blaster complements your treatment plan with non-invasive light therapy
Traditional Care Alone
- Lengthy healing periods (6-14+ weeks)
- Frequent clinic visits required
- High recurrence rates
- Does not address underlying circulation issues
- Limited at-home treatment options
Enhanced with Wound Blaster
- Up to 85% faster wound closure
- Simple 5-10 minute daily sessions at home
- 80% reduction in new wound occurrence
- Directly improves local blood circulation
- Non-invasive, pain-free treatment
Prevention Is Possible
A landmark 2004 study by Powell, Carnegie, and Burke demonstrated that infrared light therapy prevented 80% of expected new diabetic foot wounds. Of 68 high-risk patients, only 1 (1.5%) developed a new wound — compared to the expected 7.3% rate.
By restoring protective sensation through improved circulation, Wound Blaster helps diabetic patients avoid the devastating cycle of ulcer formation, infection, and recurrence.
Learn About PreventionFrequently Asked Questions
Common questions about Wound Blaster for diabetic ulcers
Can Wound Blaster be used on open diabetic ulcers?
Wound Blaster should always be placed over a bandage, never directly on an open wound. The device delivers its therapeutic LED light energy through the bandage to increase local circulation at the wound site. This gentle, non-invasive approach supports the body's natural healing process while maintaining proper wound protection. Always consult your healthcare provider for guidance on incorporating Wound Blaster into your treatment plan.
How often should I use Wound Blaster for a diabetic ulcer?
The recommended protocol is 5-10 minutes daily, applied directly to the wound area. Consistency is key for optimal results. Your healthcare provider may adjust the frequency based on your specific condition.
Is Wound Blaster a replacement for standard wound care?
No. Wound Blaster is designed to complement your existing wound care regimen, not replace it. Continue following your healthcare provider's guidance for wound cleaning, dressing changes, off-loading, and blood sugar management.
How quickly can I expect to see results?
Results vary based on wound severity, overall health, and compliance with the treatment protocol. Clinical studies have shown measurable improvements in wound closure rates. Many patients report noticeable progress within the first few weeks of consistent use.
Is the treatment painful?
No. Wound Blaster delivers gentle, non-coherent LED light energy. The treatment is completely non-invasive and pain-free. Most patients feel only a mild, comfortable warmth during the session.
Take the Next Step in Diabetic Wound Care
Join thousands of patients experiencing faster, more comfortable wound closure with clinically-backed LED light therapy.